Pregunta cualquier cosa sobre investigación
Busca artículos, consulta evidencia y obtén comentarios de expertos en un solo lugar
ACC 2026 Late-Breaking Trials
Live trial results, expert commentary, and discussion with 10+ trial authors
Feed de investigación
Investigación destacada hoy
Artículos de todas las revistas, en un solo lugar
2w ago
Comentario expertoRevista destacadaDestacado en Circulation
Level 2: RCT
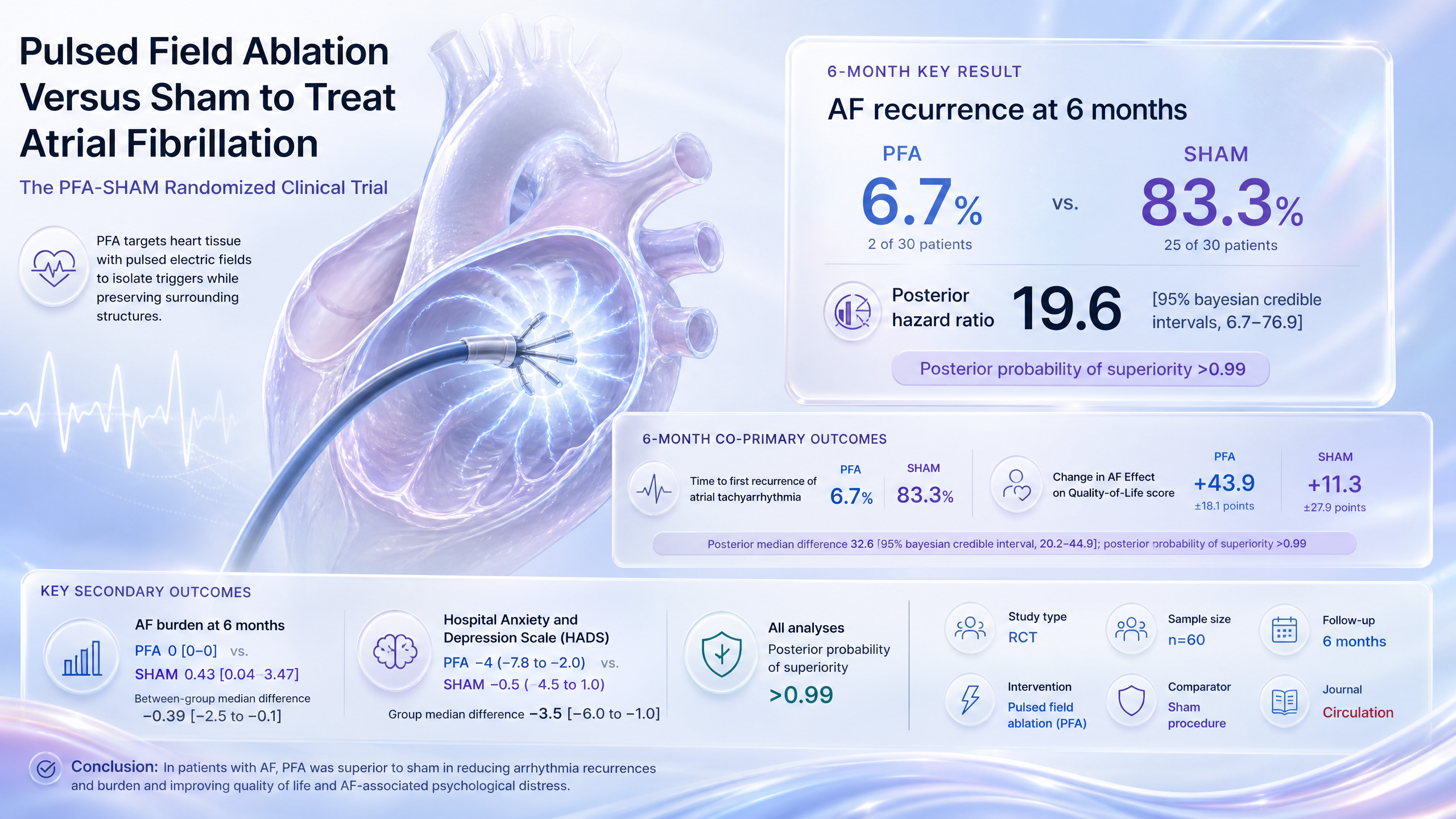
Pulsed Field Ablation Versus Sham to Treat Atrial Fibrillation: The PFA-SHAM Randomized Clinical Trial
Pulsed field ablation cuts 6-month atrial tachyarrhythmia recurrence by ~92% versus sham.
Implicación
PFA markedly outperforms sham for AF recurrence and QoL; confirms ablation benefit beyond placebo in symptomatic patients.
Circulation
Charles University
1w ago
Comentario expertoRevista destacadaDestacado en Circulation
Level 1: Clinical Guideline
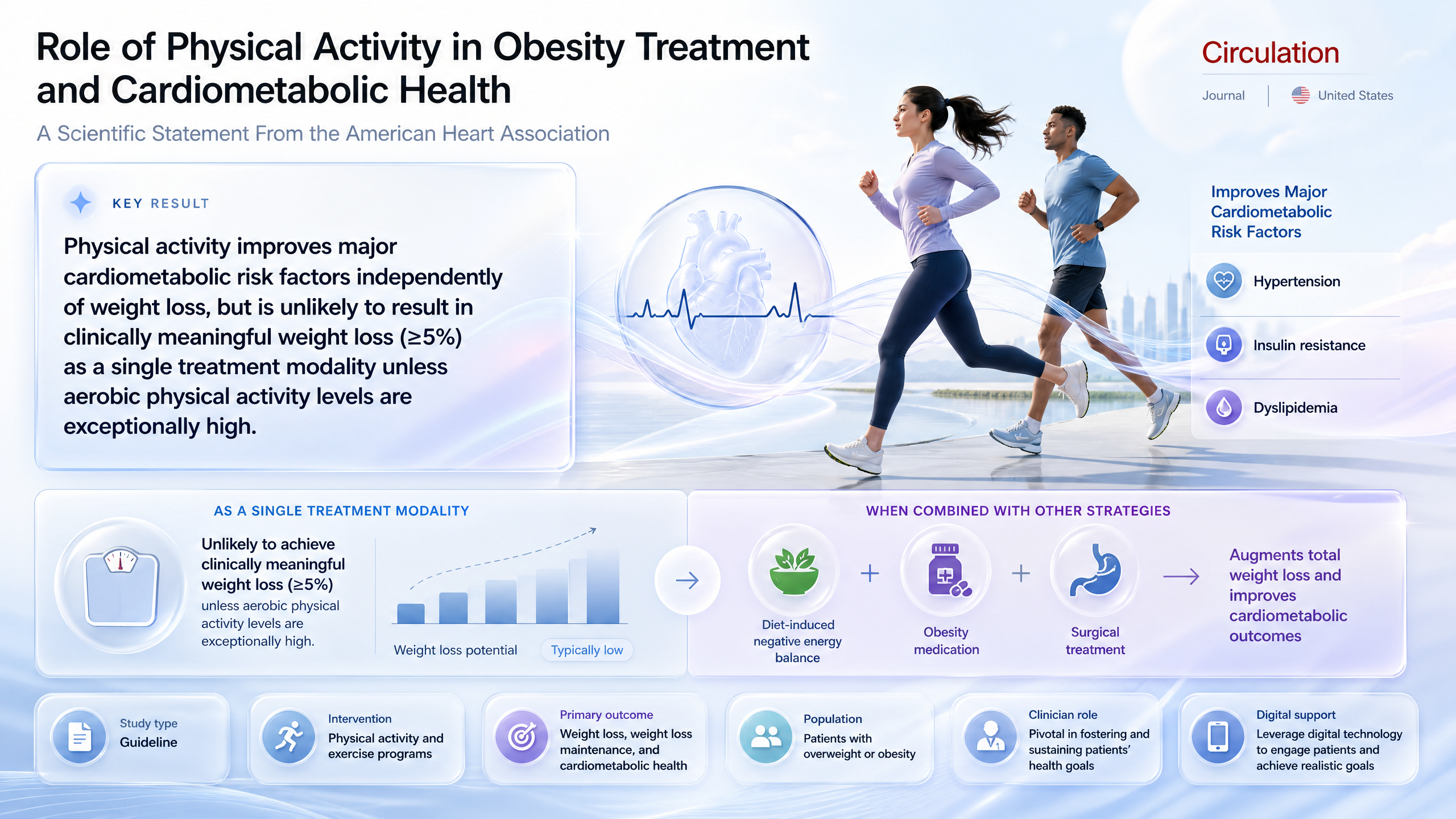
Role of Physical Activity in Obesity Treatment and Cardiometabolic Health: A Scientific Statement From the American Heart Association
Implicación
Prescribe physical activity for cardiometabolic gains irrespective of weight loss; extends evidence for multimodal obesity management.
Circulation
4w ago
Tendencia en XComentario expertoRevista destacadaDestacado en Circulation
Level 2: RCT
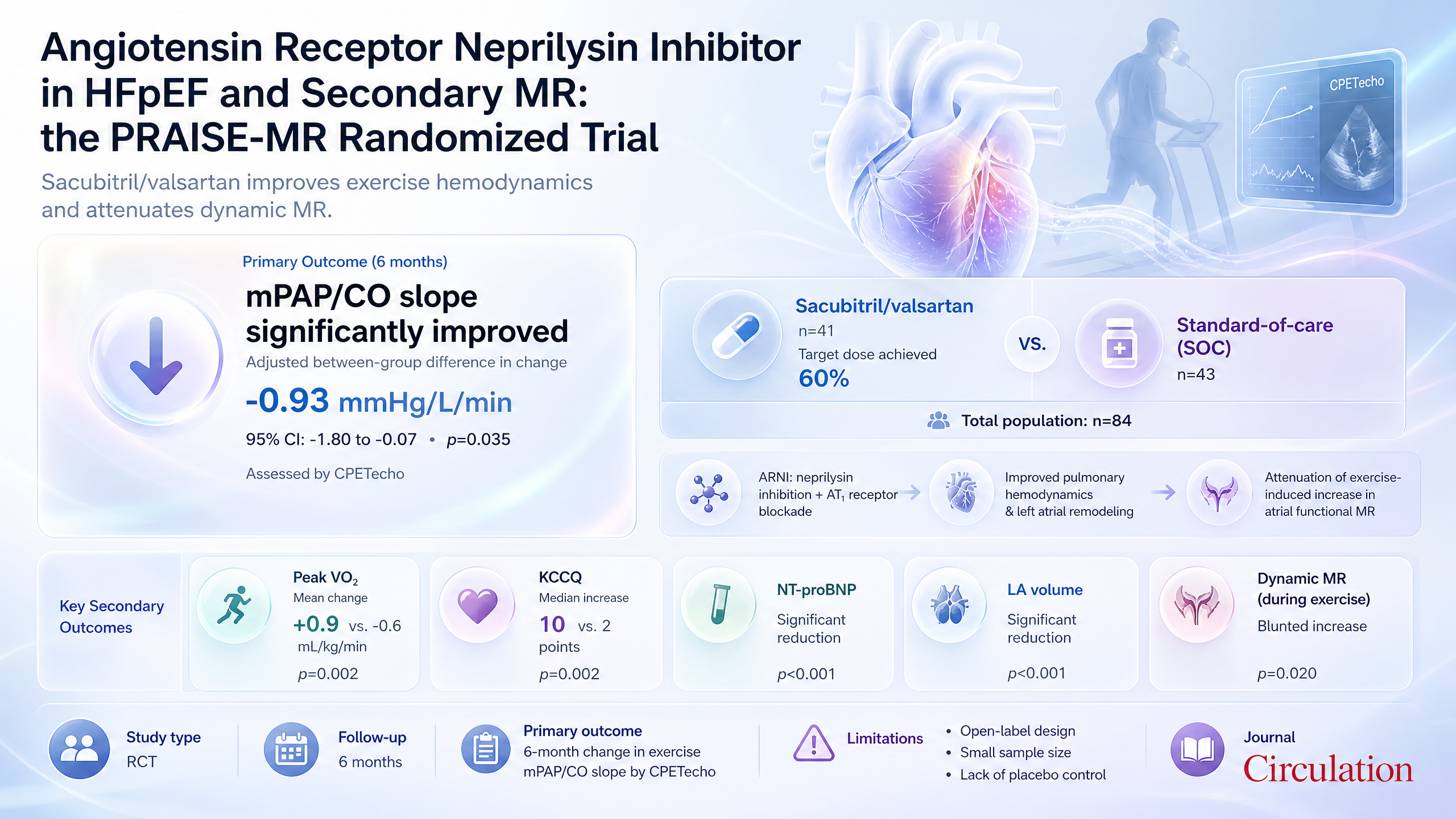
Angiotensin Receptor Neprilysin Inhibitor in Heart Failure with Preserved Ejection Fraction and Secondary Mitral Regurgitation: the PRAISE-MR Randomized Trial
Sacubitril/valsartan improves exercise mPAP/CO slope by ~0.93 mmHg/L/min versus SOC in HFpEF with AFMR.
Implicación
Supports sacubitril/valsartan over SOC in HF with adverse exercise hemodynamics; extends prior ARNI trials to this invasive endpoint.
“The PRAISE-MR trial is the first prospectively randomized trial to demonstrate that sacubitril/valsartan significantly improves exercise hemodynamics, functional capacity, and quality of life in patients with HFpEF and AFMR. These findings underscore that the phenotypic heterogeneity of HFpEF nec...”
— ACC Journal ScanVer fuente
Circulation
Vrije Universiteit Brussel
2w ago
Comentario expertoRevista destacadaDestacado en ESC Press Release
Level 1: Clinical Guideline
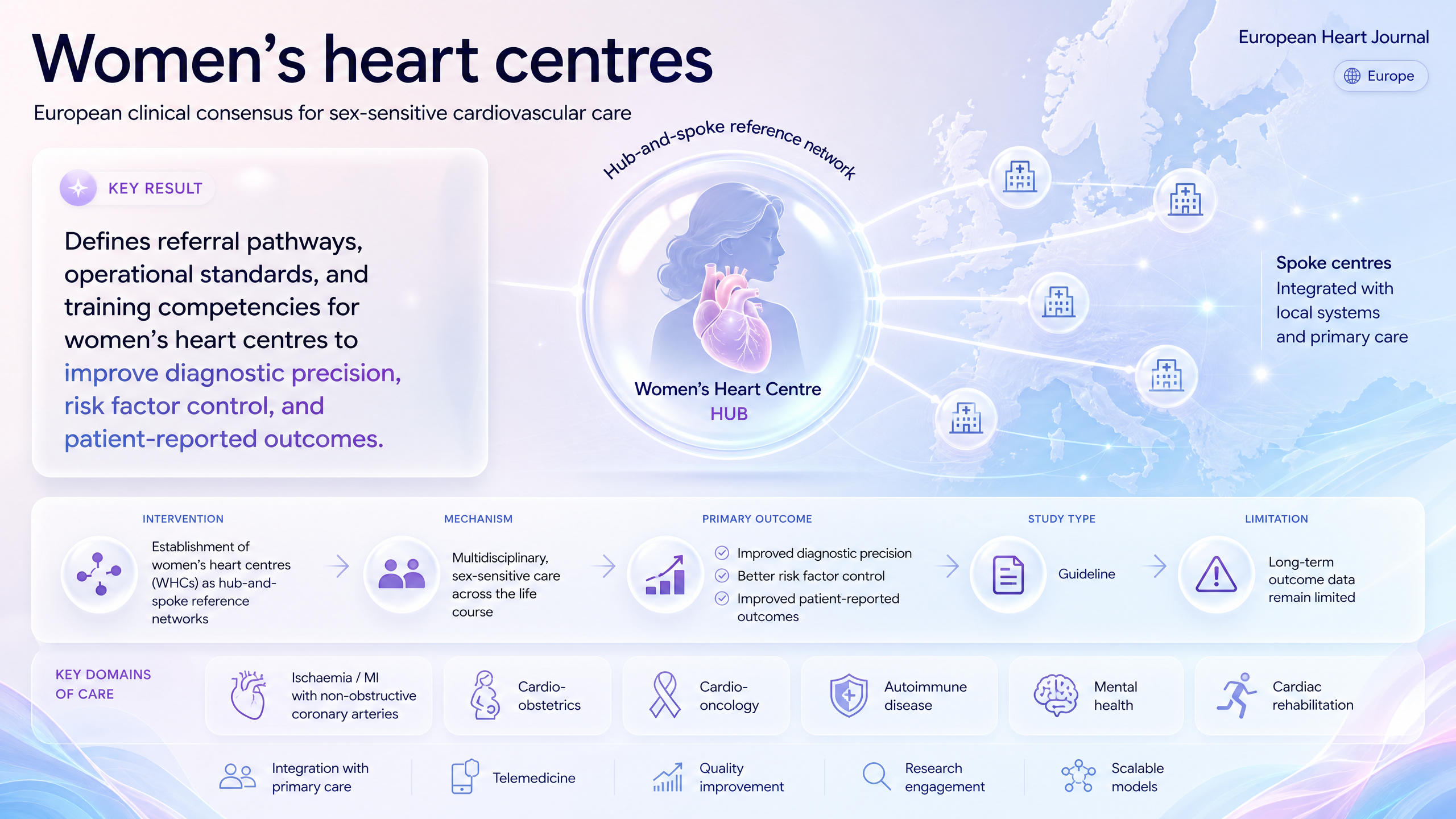
Women's heart centres: a clinical consensus statement of the European Association of Cardiovascular Imaging (EACVI), the European Association of Percutaneous Cardiovascular Interventions (EAPCI), the Heart Failure Association (HFA), and the Association for Acute CardioVascular Care (ACVC) of the ESC
Implicación
Supports women's heart centre implementation to reduce sex-based care gaps; extends consensus on specialized pathways and training.
European Heart Journal
Harvard University
1w ago
Tendencia en XRevista destacadaDestacado en ACC Journal Scan
Level 1: Meta-Analysis
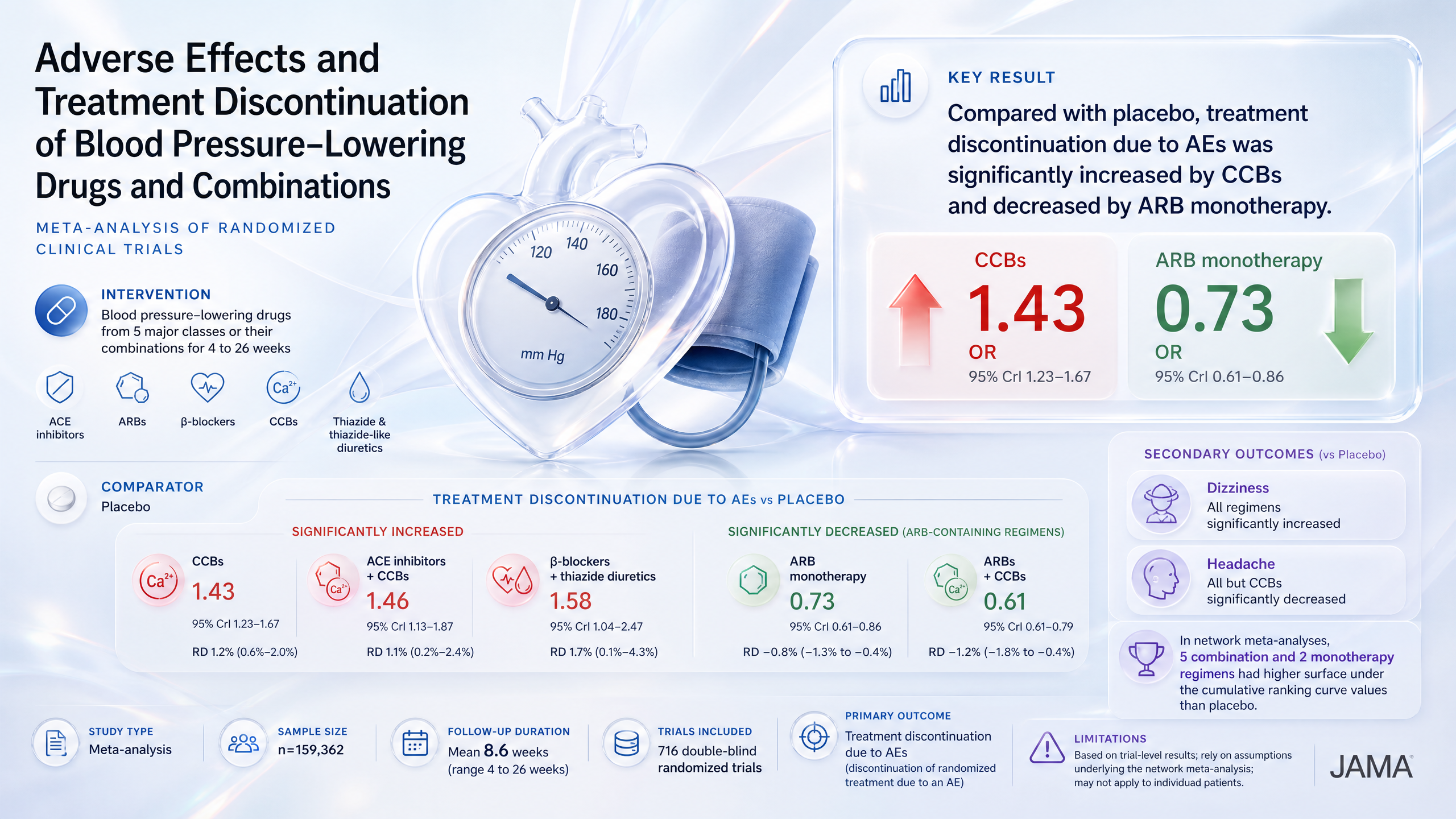
Adverse Effects and Treatment Discontinuation of Blood Pressure–Lowering Drugs and Combinations
CCBs increase adverse event discontinuations ~43% versus placebo while ARB monotherapy reduces them.
Implicación
CCBs raise and ARBs lower adverse-event discontinuations versus placebo; extends class-specific tolerability data to inform initial antihypertensive selection.
“Results from the study by Wang, et al., can help inform clinicians' selection of antihypertensive therapies for patients initiating medications for hypertension, particularly when comorbidities, such as the presence of diabetes with microvascular disease, do not warrant a specific therapy.”
— ACC Journal ScanVer fuente
JAMA
University of Oxford
1w ago
Revista destacada
Level 1: Meta-Analysis
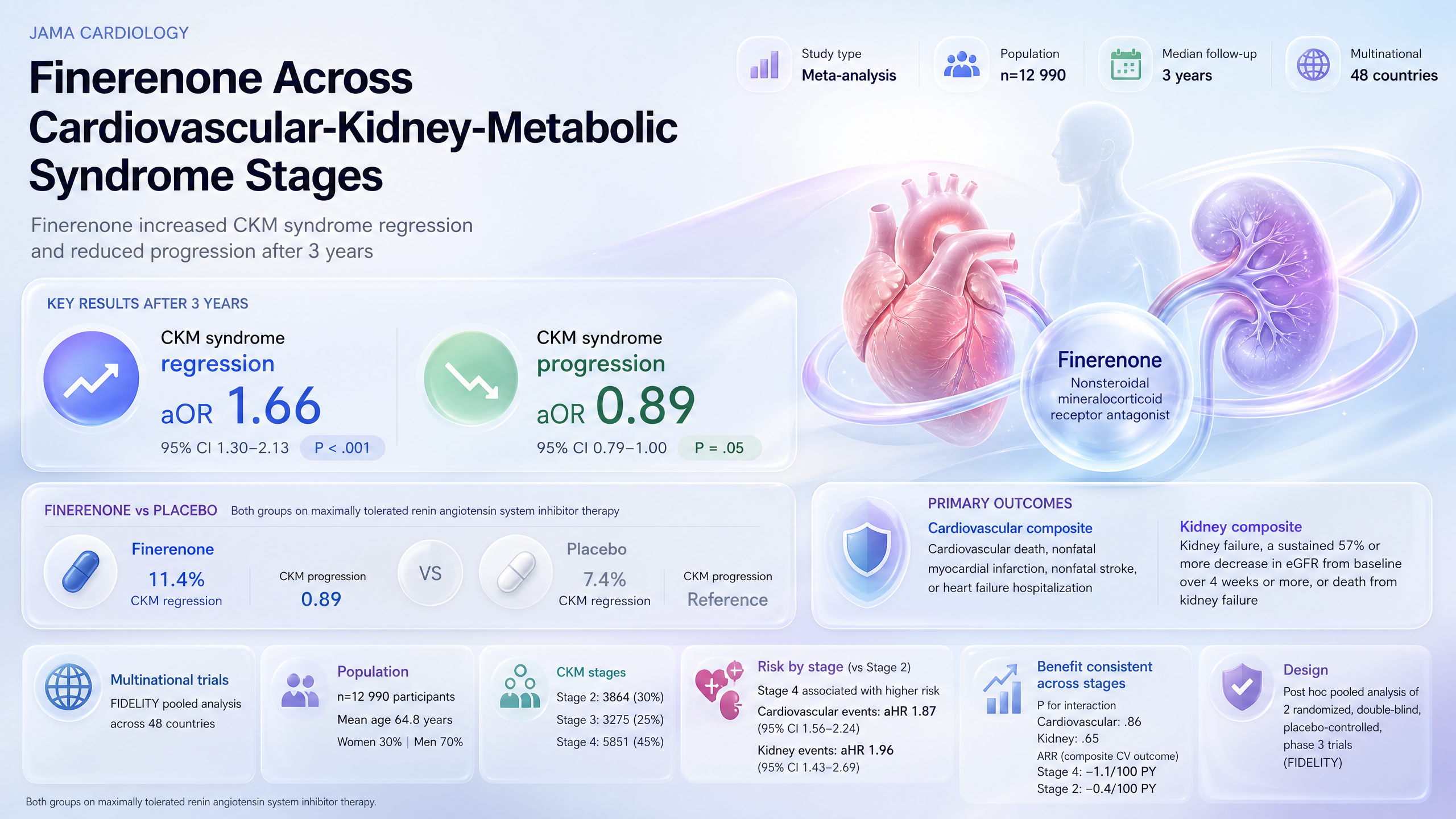
Finerenone Across Cardiovascular-Kidney-Metabolic Syndrome Stages
Finerenone reduced cardiovascular and kidney events across CKM stages and increased CKM syndrome regression (11.4% vs 7.4%; aOR 1.66; 95% CI 1.30-2.13; P<.001) compared with placebo.
Implicación
Supports finerenone across CKM stages in T2D-CKD; extends prior RCTs to include syndrome regression.
“Importantly, participants who experience new-onset AFib/AFL were at a substantially higher subsequent risk of adverse cardiovascular and kidney outcomes than were those who remained free of AFib/AFL during follow-up. These findings highlight the role of finerenone in reducing the risk of new-onset AFib/AFL, mitigating downstream complications, and ultimately improving outcomes in patients across the CKM spectrum.”
— Dr. Maria A. PabonVer fuente
JAMA Cardiology
University of Michigan
1w ago
Revista destacada
Level 2: RCT
Precardioversion Heart Rhythm Monitoring Using Smartphone Photoplethysmography
Precardioversion monitoring using smartphone photoplethysmography significantly reduced same-day cancellations of scheduled cardioversions compared to standard care (4.8% vs 23.2%; P<.001).
Implicación
Reduces same-day cancellations and resource waste in AF cardioversion; extends smartphone photoplethysmography evidence to preprocedural monitoring.
JAMA Cardiology
Karolinska Institutet

4w ago
Comentario expertoRevista destacadaDestacado en ACC Journal Scan
Level 3: Cohort Study
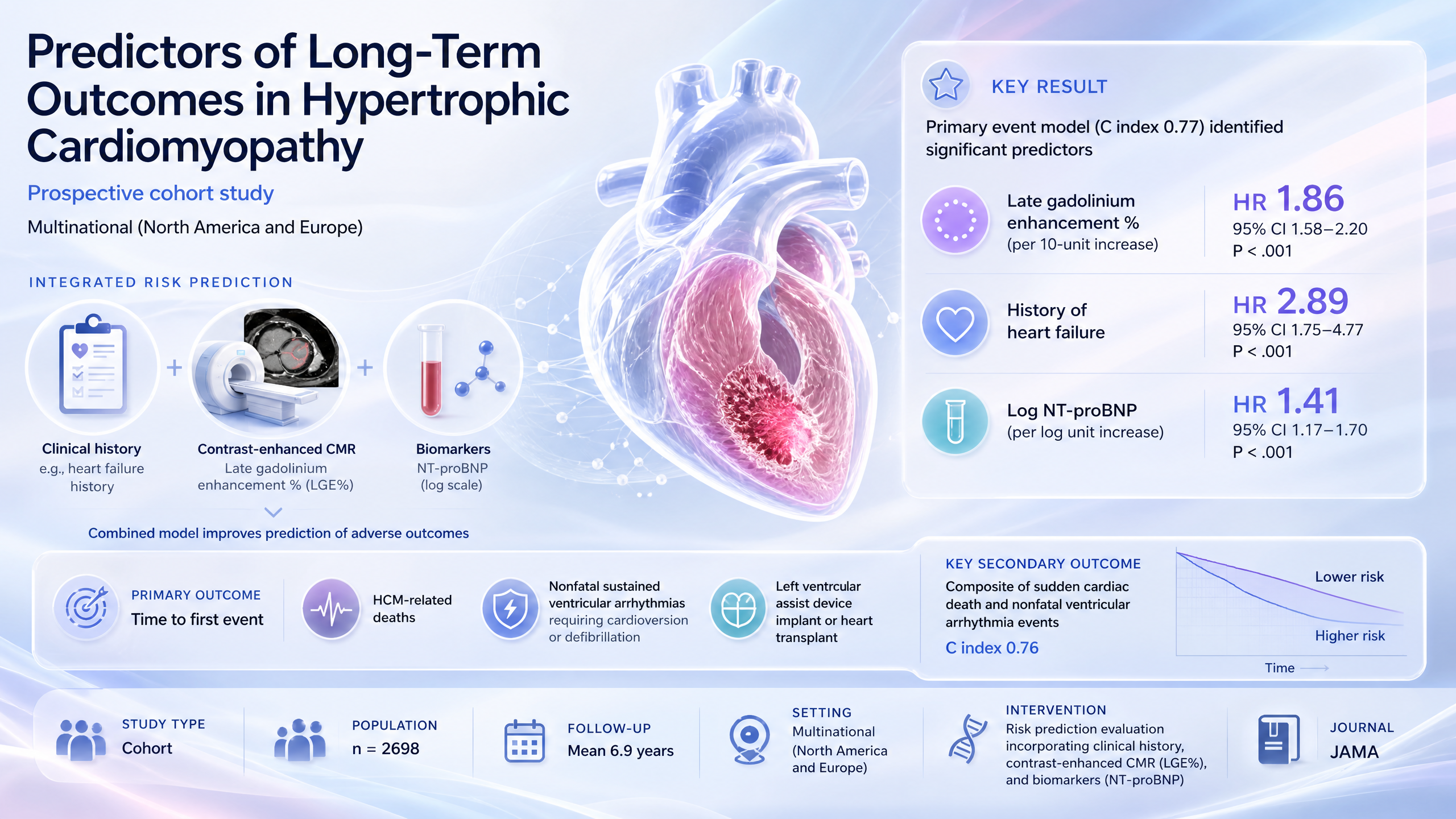
Predictors of Long-Term Outcomes in Hypertrophic Cardiomyopathy
CMR LGE% predicts ~86% higher adverse event risk in HCM, alongside NT-proBNP.
Implicación
LV scar burden by LGE may refine HCM risk stratification; this observational link extends prior markers but leaves open prospective validation before guiding therapy.
“This is an important next step to do a better job of identifying HCM patients at high risk," he said. "This adds to presently used risk markers derived from the patient's and their family's prior history.”
— ACC Journal ScanVer fuente
JAMA
University of Michigan
4w agoOpen Access
Destacado en podcastRevista destacadaDestacado en ACC Journal Scan
Level 2: RCT
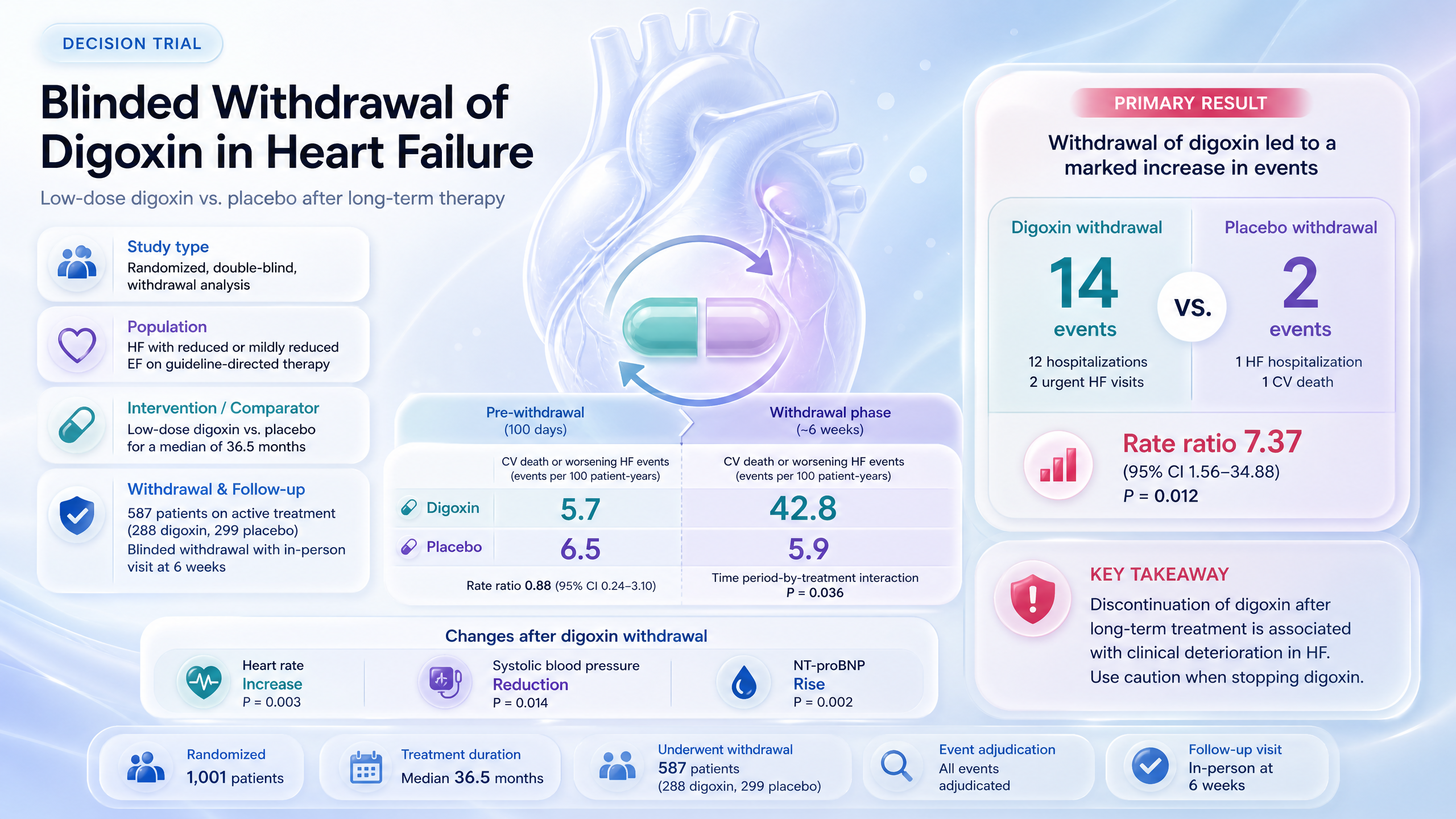
Blinded withdrawal of randomized treatment with low-dose digoxin or placebo in patients with heart failure: the DECISION trial
Withdrawing low-dose digoxin increases CV death or worsening HF events ~637% vs placebo.
Implicación
Caution against digoxin withdrawal in stable HF; confirms ongoing benefit of continued therapy.
“Discontinuation of long-term low-dose digoxin is associated with clinical deterioration of patients with chronic [HF] and a [LVEF] <50%. These findings warrant caution when stopping low-dose digoxin.”
— ACC Journal ScanVer fuente
European Heart Journal
University of Amsterdam
4w agoOpen Access
Destacado en podcastComentario expertoRevista destacadaDestacado en Circulation
Level 3: Blinded Trial
Determining the Physiological Threshold for Angina (ORBITA-FIRE): A Double-Blind, Randomized, Placebo-Controlled Study
Physiological angina thresholds vary with cardiac workload and fall consistently below universal ischemia-based limits.
Implicación
Clinicians should caution against universal ischemic thresholds for revascularization; leaves open personalized symptom-linked targets pending outcome trials.**[[1]](https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.125.078738)[[1]](https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.125.
Circulation
University College London
